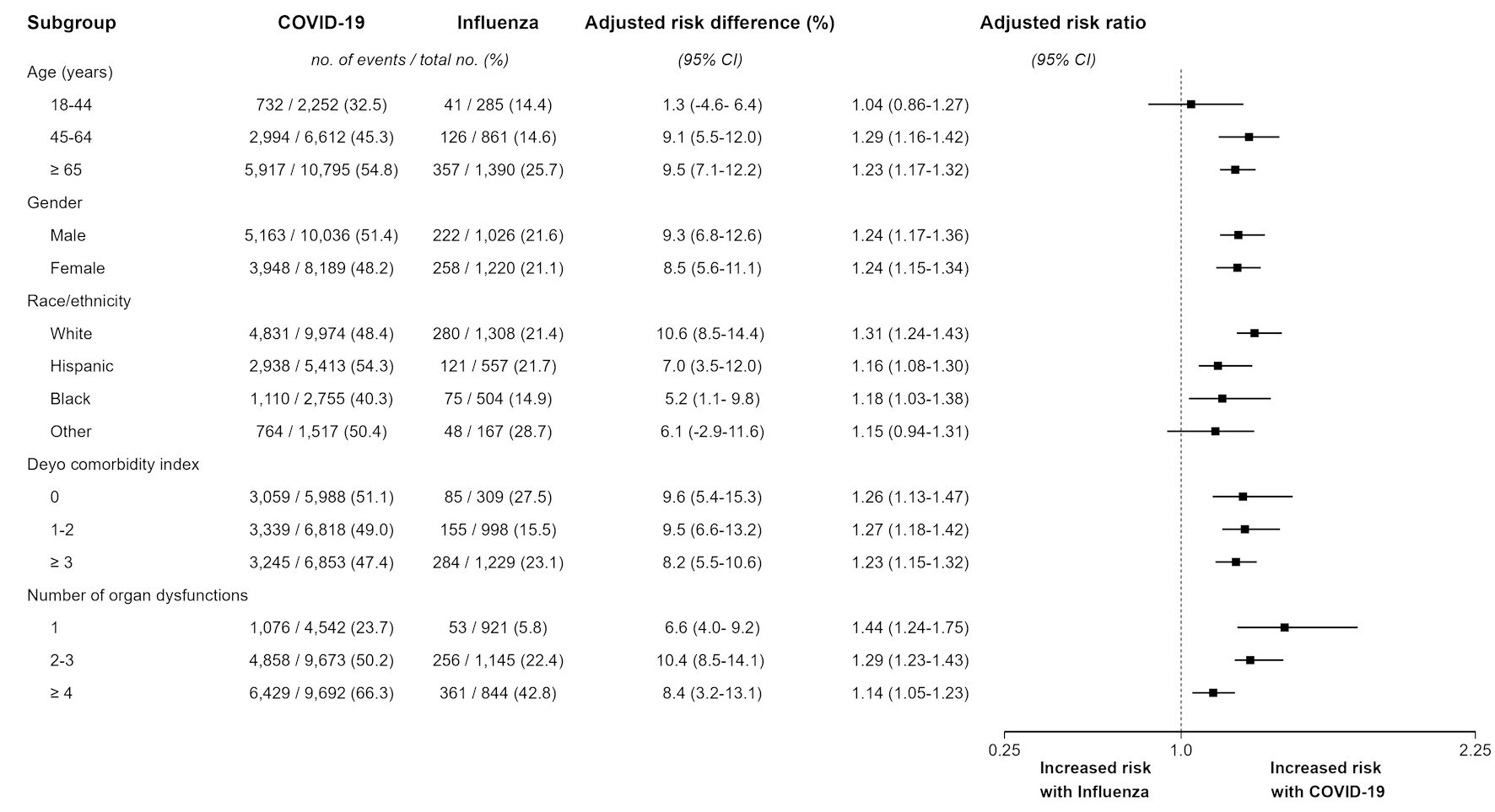
↓ Figure 1. Subgroup analysis of comparative
short-term mortality among mechanically ventilated hospitalizations with COVID-19 and influenza.
Analyses were conducted using overlap propensity score weighting. Adjusted risk ratio represents the
risk of short-term mortality among mechanically ventilated hospitalizations with COVID-19 compared to
those with influenza. Adjusted risk difference represents the absolute difference in short-term
mortality among mechanically ventilated hospitalizations with COVID-19 compared to those with influenza,
expressed as percentage. Non-parametric bootstrap 95% confidence intervals (CIs) were determined using
10,000 bootstrap samples and the percentile method. The width of the CIs was not adjusted for
multiplicity and should not be used to infer definite effects. COVID-19: coronavirus disease 2019.